Table of Contents
Cavities Definition
Cavities are permanently damaged areas on the surface of your teeth that develop into small openings or holes. It occurs due to a combination of factors, such as bacteria in the mouth, frequent snacking, sugary drinks, and low dental cleaning.
Dental cavities are one of the most shared health problems in the world. They appear significantly often in children, adolescents, and older adults. However, all people who have teeth can get cavities, even babies.
If left untreated, cavities can spread and affect deeper layers of the teeth. They can cause severe toothache, infection, and tooth loss. The best protective measures against tooth decay are regular dental visits and good brushing and flossing habits.
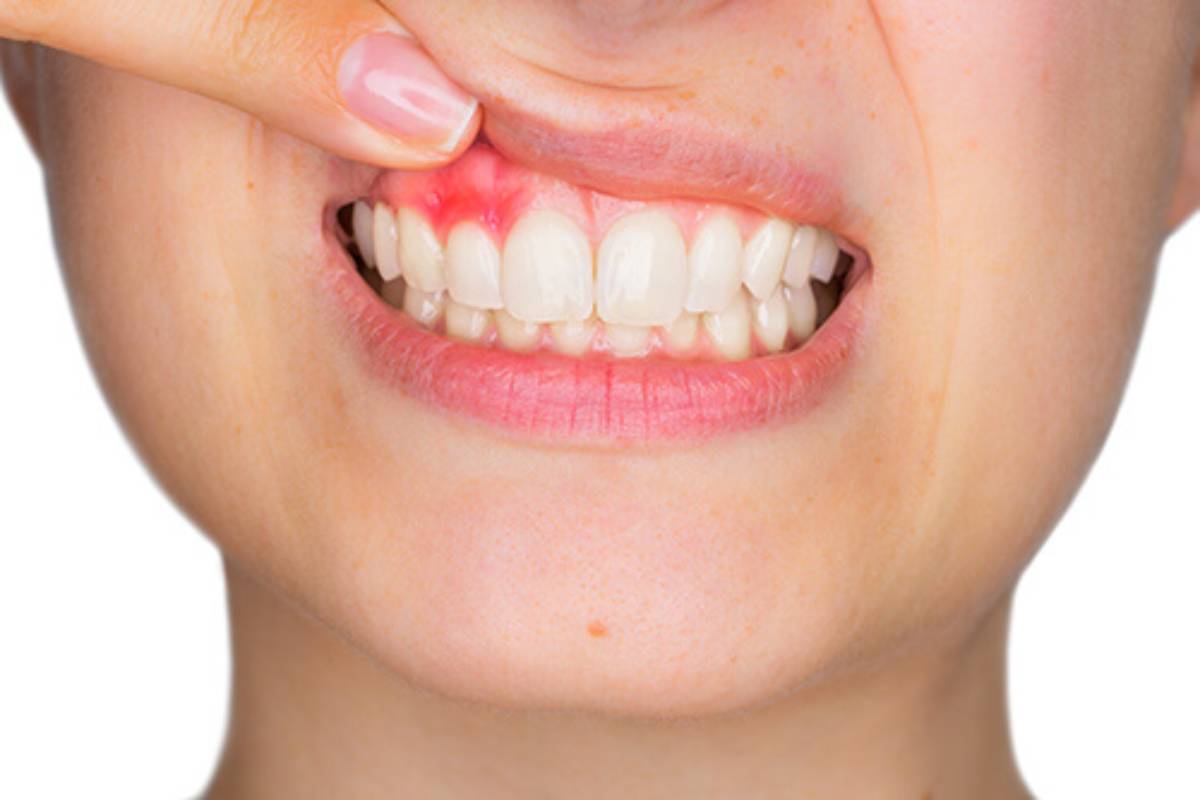
What are the Symptoms of Cavities?
The signs and symptoms of cavities vary, contingent on the size and location. When a hole begins to form, you may not have any symptoms. As tooth decay rises in size, it can reason signs and symptoms, such as the following:
- Toothache, sudden pain, or pain that happens for no apparent reason;
- Tooth sensitivity;
- Mild to shrill pain when you eat or drink something sweet, hot, or cold;
- Visible holes or depths in teeth;
- Brown, black, or white stain on any surface of a tooth;
- Pain when you bite.
Causes of Cavities
Tooth decay is a process that happens over time. It is how tooth decay forms:
1. Plaque Formation
- Dental plaque is a sticky transparent film that coats your teeth. It is generated by consuming a lot of sugars and starches and not brushing your teeth well.
- When sugars and starches not clean from teeth, bacteria quickly begin to feed on them and form plaque.
- Plaque that remains on teeth can harden below or above the gum line and turn into tartar.
- Tartar makes it difficult to remove plaque and creates protection for bacteria.
2. Plaque Attacks
- Plaque acids remove minerals from the hard, outer enamel of the teeth. This erosion reasons tiny openings or holes in the enamel, the first stage of cavities.
- Once parts of the enamel worn away, bacteria and acid reach the next layer of the teeth, called ‘dentin.’
- This layer is laxer than coating and fewer resistant to acid. Dentin has small tubes that communicate straight with the tooth’s nerve and cause sensitivity.
3. The Destruction Continues
- As tooth decay methods, bacteria and acid continue their journey through the teeth, then moving into the tooth’s material (pulp) that covers nerves and blood vessels.
- The pulp becomes inflamed and angry by microorganisms. Since there is no room for irritation to enlarge inside a tooth, the nerve becomes pinched, causing pain.
- The discomfort can even extend outside the root of the tooth, towards the bone.
Risk Factors of Cavities
Everybody who has teeth is at risk for cavities, although the following factors may increase the chances:
1. Tooth Location
- Cavities almost always appear on the spinal teeth (molars and premolars). These teeth have numerous grooves, holes, cracks, and multiple roots that can collect food particles.
- As a result, it is more stimulating to keep them clean than the front teeth, which are smoother and more comfortable to reach.
2. Certain Foods and Drinks
- Foods that twig to teeth for a long time like milk, ice cream, honey, sugar, soda, nuts, cake, cookies, hard candy, mints, cereals.
- Dried potatoes and French fries are more likely to cause cavities than those easily removed by saliva.
3. Eat or Drink Frequently
- By constantly snacking or consuming sugary drinks, you feed the bacteria in your mouth more food to produce acids that attack and wear down your teeth.
- Also, drinking soda and other acidic beverages throughout the day helps create a continuous acid layer on your teeth.
4. Feeding Babies Before Bed
- When babies beverage bottles of milk, formula, juice, or other sugary fluids before bed, those drinks stay on their teeth for hours while babies sleep, feeding the bacteria that cause cavities.
- This damage is often called “bottle tooth decay.” Similar damage can occur when young children were pacing around while drinking these beverages from a spouted glass.
5. Inadequate Brushing
- If you don’t brush your teeth quickly after eating and consumption, plaque builds up quickly, and the early stages of tooth decay can start to appear.
- The recommended brushing time is two minutes. If you’re brushing less than that, then you’re not cleaning your oral cavity properly.
- Inappropriate brushing techniques can also lead to cavities. Remove plaques by applying the right brushing technique. The toothbrush must be in a 45-angle position to your gums. Brush your teeth by moving the brush back and forth using short strokes. Make sure to brush all tooth surfaces, including the inner and outer areas.
6. Lack of Fluoride
- Fluoride, a naturally occurring mineral, aids prevent cavities and even reverse the early tooth damage stages.
- Due to its aids for the teeth, fluoride adds too many water supplies.
- It is also a standard component of toothpaste and mouthwashes. However, bottled water generally does not contain fluoride.
7. Age
- In the United States, cavities are joint in young children and teens. Older adults are also at a greater danger of having them.
- Over the period, teeth may wear out, and gums retract, making teeth more vulnerable to tooth-root decay.
- Older adults can take medications that decrease salivation, which increases the risk of cavities.
8. Dry Mouth
- A dry mouth produced by a lack of saliva assists prevents cavities by removing food and plaque from your teeth.
- Substances in saliva also assistance counteract the acid shaped by bacteria.
- Some medications, some diseases, radiation to the skull or neck, and certain chemotherapy drugs can upsurge the risk of tooth decay by decreasing saliva production.
9. Worn Fillings or Dental Devices
- Over the years, fillings can weaken, begin to break or form rough edges. It allows plaque to build up more quickly and makes it difficult to remove.
- Dental appliances can become out of adjustment, allowing cavities to start to form under them.
10. Heartburn
- Heartburn or gastroesophageal reflux disease can reason stomach acid to move up into the mouth (reflux), causing the enamel to wear down and causing significant teeth damage.
- It exposes more of the dentin to attack by bacteria and creates cavities.
- Your dentist may recommend that you see your doctor to see if gastric reflux is the cause of enamel loss.
11. Eating Disorders
- Anorexia and bulimia can be principal to tooth erosion and significant cavities.
- The stomach acid from repeated vomiting (purging) coats the teeth and begins to dissolve the enamel.
- Eating disorders can also delay saliva production.
Complications of Cavities
Tooth decay is so mutual that you might not care about it. You may reason that it doesn’t matter if children have cavities in their baby teeth. However, tooth decay can have severe and long-lasting complications, even for those children who do not yet have permanent teeth.
Complications of cavities can include:
- Pain;
- Dental abscess;
- Swelling or pus around a tooth;
- Broken or damaged teeth;
- Chewing problems;
- The changes in tooth position after losing a tooth.
- When cavities are severe, you may have:
- Pain that interferes with daily life;
- Weight loss or nutrition difficulties such as pain or trouble eating or chewing;
- Loss of teeth, which can move appearance, confidence, and self-esteem;
- In rare cases, a tooth abscess (a pocket of pus caused by a bacterial infection) can lead to more severe or even life-threatening illnesses.
Prevention of Cavities
Good oral hygiene can help you stop tooth decay. Here are some tips to assistance prevent cavities. Ask your dentist which instructions are best for you.
1. Brush with Fluoride Toothpaste Afterwards Eating or Drinking
- Brush your teeth at the smallest double a day and ideally after every meal, with a toothpaste covering fluoride.
- Use dental floss or an interdental detergent to clean between your teeth.
2. Rinse your Mouth
- If your dentist thinks you are in danger of cavities, they may recommend that you use a fluoride mouthwash.
- Gargling with hydrogen peroxide can help disinfect the mouth to prevent and treat cavities. Don’t worry because hydrogen peroxide is safe and good for your oral health. The safety of hydrogen peroxide comes from its natural ingredients, which are oxygen and water. This solution can also help reduce inflammation and brighten your teeth.
- See your Dentist Regularly
- Get expert dental cleanings and regular oral exams. These can assist you to prevent problems or detect them early.
- Your dentist can recommend a schedule that is correct for you.
4. Consider using Dental Sealants
- A sealant is a defensive plastic coating that applies to the chewing surface of the back teeth.
- Seals grooves and cracks that tend to accumulate food, protecting tooth coating from plaque and cutting.
- The Centers for Disease Control and Prevention (CDC) commends using sealants for all school-age children.
- While sealants can last for numerous years before they need to replace, they need to check regularly.
5. Drink Some Tap Water
- Most public water networks contain fluoride, which can help reduce tooth decay significantly.
- If you only beverage bottled liquid that does not comprise fluoride, you will miss out on fluoride benefits.
6. Avoid Eating or Drinking Frequently
- When you eat or drink beverages other than water, you help bacteria in your mouth crop acids that can finish tooth enamel.
- If you eat or drink throughout the day, your teeth are in constant attack.
7. Eat Healthy Foods for your Teeth
- Some foods and drinks are healthier for your teeth. Avoid foods that can get wedged in the grooves and pits of your teeth for long periods, or brush soon after eating.
- However, foods like fresh fruits and vegetables increase saliva flow; coffee, unsweetened tea, and sugar-free gum help clean food particles.
- Apply Good Oral Practices
- Don’t use your teeth for opening bottles, tearing plastics, or any other purposes except for eating.
- Avoid biting too hard on food, including ice cubes and candies. In addition, avoid eating hard-to-chew food as much as possible.
Diagnosis of Cavities
In general, the dentist can easily detect cavities by:
- Question about toothache and sensitivity
- Examine the mouth and teeth
- Scan teeth with dental instruments for soft spots
- Look at dental X-rays, which can show the degree of decay and decay.
- Your dentist can also tell you which of the three types of cavities you have: soft surface, pit, fissure, or root.
Treatment of Cavities
Regular examinations can identify cavities and other dental diseases before they cause troublesome symptoms and lead to more severe problems. The earlier you try to find medical attention, the more likely you will reverse the early stages of tooth decay and prevent its progression. If a cavity treats before it starts to cause pain, you probably won’t need long-term treatment.
The treatment of cavities depends on the severity and your particular situation. Some treatment options are as follows:
1. Fluoride Treatments
- If a cavity is beginning to appear, fluoride treatment can help restore tooth enamel and sometimes reverse cavities in very early stages.
- Professional fluoride treatments contain more fluoride than is found in tap water, toothpaste, and mouthwashes.
- Fluoride treatments can be liquid, gel, foam, or varnish brushed on the teeth or placed in a small tray that hysterics over the teeth.
2. Fillings
- Sometimes called “restorations,” Fillings are the primary treatment option when caries have progressed beyond the first stage.
- Fillings are made from various materials, such as tooth-colored composite resins, porcelain, or a dental amalgam that combines different materials.
3. Crowns
- If you have extensive cavities or weakened teeth, you may need a crown – a custom-made covering that replaces the tooth’s complete natural crown.
- The dentist will drill the decayed area and other parts of the tooth to ensure a good fit.
- Crowns can make gold, high-strength porcelain, resin, porcelain fused to metal, or other materials.
4. Endodontics
- When decay reaches the inside of the tooth (pulp), you may need root canal treatment.
- It is a treatment to repair and preserve a badly damaged or infected tooth instead of extracting it.
- The pulp of the diseased tooth remove. Medicines are sometimes placed in the root canal to clear the infection. The pulp then replaces with a filling.
5. Tooth Extraction
- Some teeth have such severe cavities that they cannot restore and must remove.
- Tooth extraction can leave a gap that causes the other teeth to shift. If possible, consider getting a bridge or dental implant to replace the missing tooth.
When to See the Dentist
You may not notice that a cavity is forming. That’s why it’s essential to get regular dental checkups and cleanings, even when your mouth is delicate. However, see your dentist as soon as likely if you experience a toothache or pain in your mouth.
Toothache or oral pain is a good example of a dental emergency. Neglecting toothache may result in more complications in the long run. While the pain may subside when you take pain medication, the real cause of the problem is only masked, which could lead to deeper cavities or gum disease.
Conclusion
Your oral health touches more than just your teeth. Poor oral and dental health can donate to subjects with your self-esteem, speech, or nutrition.
They can also affect your ease and overall quality of life. Many dental and oral problems grow without any symptoms. Seeing a dentist regularly for an examination and a test is the best method to catch a problem before it gets worse.
Ultimately, your long-term outcome is contingent on your efforts. You can’t always stop every cavity, but you can decrease your danger of direct gum disease and tooth loss by remaining on top of your daily oral care.