Table of Contents
What is Folliculitis?
Folliculitis is a common skin problem, which the hair follicles become inflamed. And also bacterial or fungal infection usually causes it.
It can manifest as tiny red bumps or whiteheads around hair follicles – the little pockets from which each hair grows. And also the infection can spread and become scaly, non-curable ulcers.
The disease is not life-threatening. However, it can cause itching, pain, and embarrassment. Some infections can cause permanent hair loss and scarring.
Your case is mild, it will likely resolve itself in a few days with necessary self-care measures. And also in instances where it is more severe or recurrent, however, you may need to consult a doctor about prescription medications.
And also certain types of folliculitis know as “hot tub folliculitis,” “ingrown hair,” and “beard folliculitis.”
What are the Symptoms of Folliculitis?

The signs and symptoms of folliculitis are:
- A group of red bumps or white-headed pimples that form around hair follicles;
- Pus-filled blisters that break open and crust over;
- Itchy or burning skin;
- Pain or tenderness in the skin;
- A swollen lump or bump.
What are the Types of Folliculitis?
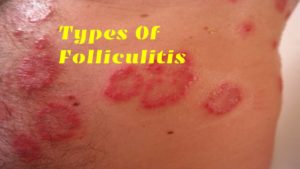
The main types of folliculitis are superficial and deep. The external type affects only a part of the follicle.
And also the deep type involves the entire hair and is usually more severe.
The Types of Superficial Folliculitis Include:
1. Bacterial Folliculitis
- White, pus-filled, itchy bumps characterize this common type.
- It occurs the hair infected with bacteria, usually Staphylococcus aureus (staph).
- Staph lives on the skin. And also it causes problems only they enter the body through a cut or other wound.
2. Hot Tub Folliculitis (Pseudomonas Folliculitis)
- With this type, you may develop a rash of red, round, itchy bumps one to two days after—a being exposed to the bacteria that causes it.
- Hot tub folliculitis causes by pseudomonas bacteria found in many places.
- As hot tubs and heated swimming pools, where chlorine and pH levels are not well regulated.
3. Ingrown Hair (Pseudofolliculitis Of The Beard)
- Firstly skin irritation caused by ingrown hairs. It mainly affects men with curly hair shaving a lot and is most noticeable on the face and neck.
- Secondly, people who wax the bikini area can develop beard folliculitis in the groin area.
- And also this condition can leave dark scars (keloids).
4. Pityrosporum Folliculitis
- Firstly this produces chronic, red, itchy bumps on the back, chest, neck, shoulders, upper arms, and also face.
- Secondly, it generates a yeast infection.
The Types of Deep Folliculitis Include:
1. Sycosis of the Beard

This type affects men who have started to shave.
2. Gram-Negative Folliculitis
Sometimes this type occurs if you are on long-term antibiotic therapy for acne.
3. Boils and Carbuncles
These occur the hair follicles become deeply infected with staph bacteria. And also usually, a boil appears, suddenly, as a painful pink or red lump. A carbuncle is a group of spots.
4. Eosinophilic Folliculitis
This type of mainly affects people with HIV / AIDS. Signs and symptoms include severe itching. And also its recurring patches of bumps and pimples form near the hair follicles on the face and upper body.
What are the Causes of Folliculitis?
- In many cases, firstly it occurs to an infection of the hair follicles by the bacteria Staphylococcus aureus (staph).
- And also it can cause by viruses, fungi, and even inflammation of ingrown hairs.
- Follicles were dense on the scalp.
- And also it occurs all parts of the body except the palms of the hands, soles of the feet, lips, and also mucous membranes.
Risk Factor’s of Folliculitis

Anyone can get it. Certain factors make you more vulnerable to the disease, including:
-Firstly having an illness that reduces your resistance to infections, like diabetes, chronic leukemia, and HIV / AIDS;
-Secondly, have acne or dermatitis;
-And also take some medication, as steroid creams or long-term antibiotic therapy for acne;
-And also being a man with curly hair who shaves;
-Frequent use of clothing that absorbs heat and sweat, like rubber gloves or high boots;
-And also taking immersion baths in hot tubs that are not well maintained;
-Damaging hair by shaving, waxing, or wearing tight clothing;
Complications
The possible complications of folliculitis are:
- Firstly reappearance or spread of infection;
- Secondly, boils under the skin (furunculosis);
- Permanent skin damage, as scars or dark spots;
- And also the destruction of hair follicles and permanent hair loss.
Preventions
These tips will help you prevent folliculitis from coming back:
- Firstly avoid tight clothing-Helps reduce friction between skin and clothing.
- Secondly, dry the rubber gloves after each use-If you wear rubber gloves regularly, turn them over after each use, wash them with soap and water, and dry them well.
- And also avoid shaving if possible-For men with ingrown hair from shaving (pseudo-folliculitis), growing a beard may be a good option if you don’t need a clean-shaven face.
- And also shave carefully-You do shave, to help control symptoms by reducing the proximity of shaving and also the risk of damaging the skin.
Treatments
- Firstly it is usually minor and goes away own without treatment.
- And also if you have skin irritation accompanied by a fever, spreading rash, or pus-filled and smelly bumps, seek medical help.
- To treat acute it that’s severe or slow to heal, your doctor may recommend over-the-counter or prescription medications.
- -Oral or topical antibiotics or antifungal medicines to treat the infection; NSAIDs or antihistamines to relieve pain or itching.
- And also chronic it can make it more challenging to treat. Antibiotics and other medicines may not clear up chronic cases.
- If additional treatment options fail, a doctor recommends laser hair removal.
- And also in treatment, stop removing hair by plucking, waxing, or shaving. Allowing your hair to grow helps your follicles to heal.
- For it, your doctor may advise you to let your hair to extend for up to three months.
Diagnosis
- To diagnose it, your doctor will examine the inflamed or irritated areas of your skin. And also be sure to tell your doctor:
- -How long you’ve had bumps on the skin; What other symptoms you’ve been experiencing; Whether you have a history of it.
- And also the doctor may diagnose it base on appearance alone. To identify the cause, they may take one of the bumps for testing.
Also Read: Tapeworm Infection – Definition, Symptoms, Causes, and More

