Table of Contents
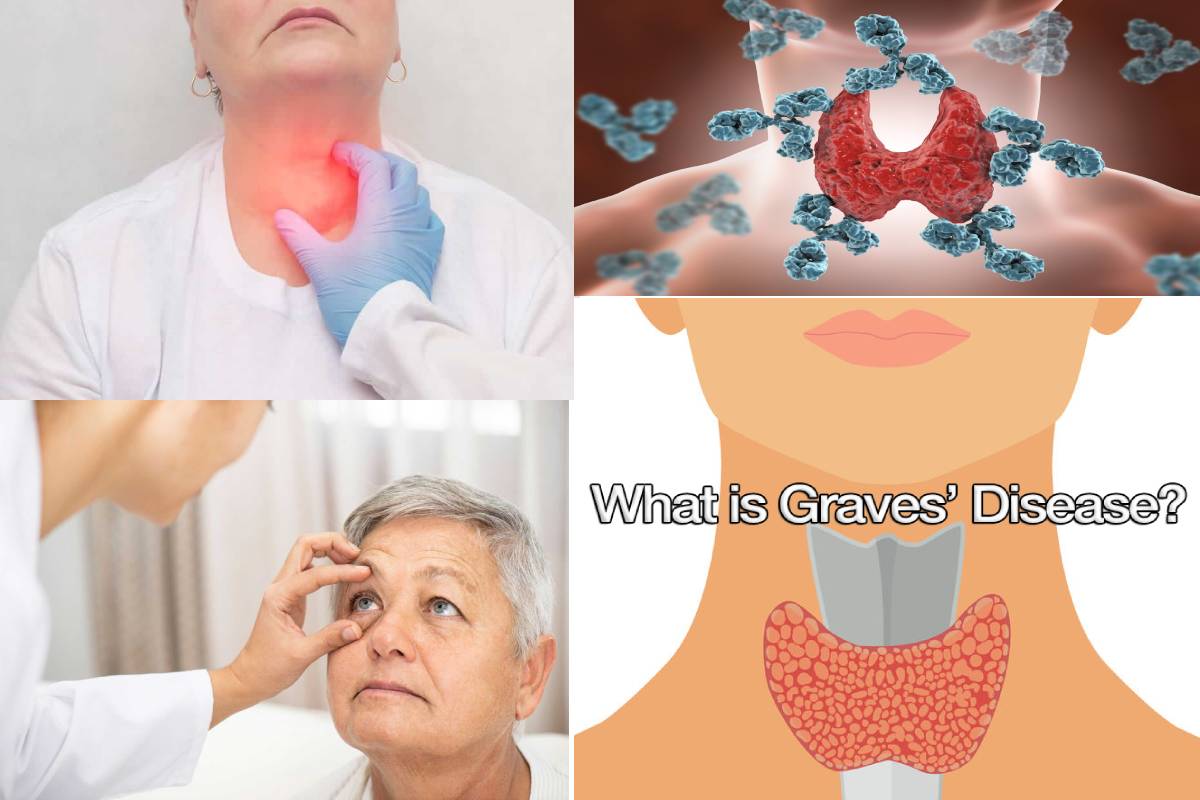
Graves’ Disease Definition
Graves’ disease is an immune system disease that affects the overproduction of thyroid hormones. Although several conditions can lead to hyperthyroidism, Graves’s disease is a common cause.
Because thyroid hormones affect several different body systems, the signs and symptoms associated with it can be diverse and significantly affect your overall well-being.
Although this disease can affect anyone, it is more common in women and before the age of 40. The primary goals of treatment are to inhibit the overproduction of thyroid hormones and decrease symptoms.
What are the Symptoms of Graves’ Disease?
- Enlarged thyroid
- Enlarged thyroid Open pop-up dialog box
- Photograph of eye complications associated with Graves’ disease
- Graves ophthalmopathy Open pop-up dialog box
- And also, Graves dermopathy
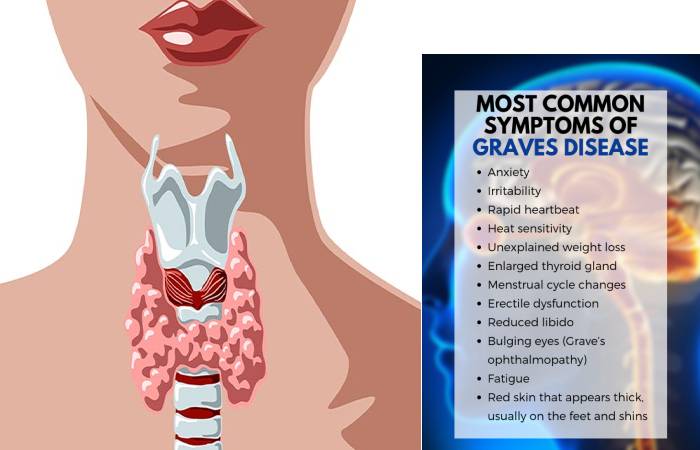
Some common signs and symptoms of Graves’ disease are:
- Anguish and irritability
- A slight tremor of the hands or fingers
- Sensitivity to heat and increased sweating, or hot, clammy skin
- Weight loss, despite regular eating habits
- Abnormal enlargement of the thyroid gland (goiter)
- Changes in menstrual cycles
- And also, Erectile dysfunction or decreased libido
- Frequent bowel movements
- Bulging eyes (Graves ophthalmopathy)
- Fatigue
- Thick, red skin, usually over the shins or tops of the feet (Graves’ dermopathy)
- Irregular or fast heartbeat (palpitations)
Causes of Graves’ Disease
- Graves disease caused a malfunction of the body’s immune system that fights infection, although it does precisely knowingly why it happens.
- The immune system’s normal response is to produce antibodies designed to attack a specific virus, bacteria, or foreign substance.
- In Graves’s disease, the body makes an antibody against part of the thyroid gland’s cells, a hormone-producing gland located in the neck, for reasons that not well understand.
- Under normal conditions, thyroid function regulates by a hormone released by a small gland at the brain (the pituitary).
- The antibody associated with this disease — thyrotropin receptor antibody — acts as the pituitary’s regulatory hormone.
- It means that the thyrotropin receptor antibody overrides the thyroid’s normal regulation and leads to thyroid hormones.
Graves’ Ophthalmopathy
- This disorder produces certain carbohydrates in the muscles and tissues located behind the eyes, the cause of which is also unknown. The same antigen that can cause thyroid dysfunction would also have an “attraction” to the tissues around the eyes.
- Graves’ ophthalmopathy usually appears at the same time as hyperthyroidism or several months later.
- But the signs and symptoms of ophthalmopathy can occur years before or after the onset of hyperthyroidism. Graves’ ophthalmopathy can also appear even without hyperthyroidism.
Grave’s Eye Disease
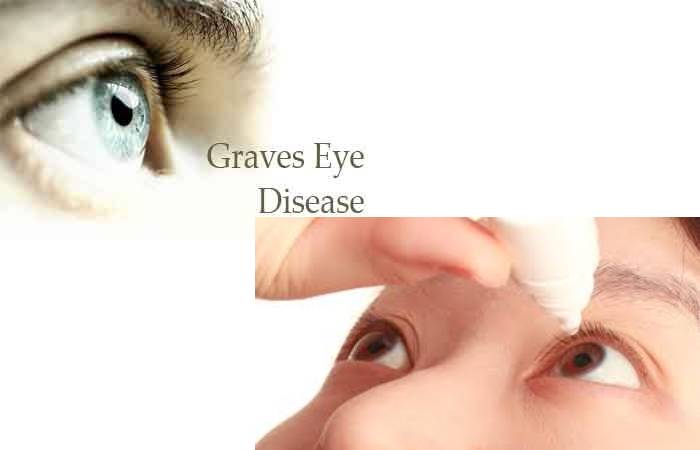
About 30 percent of people with Graves disease also have signs and symptoms of a disorder known as Graves’ ophthalmopathy.
Graves’ ophthalmopathy, inflammation, and other signs of the immune system affect the muscles and other tissues around the eyes. The resulting signs and symptoms can be:
- Bulging eyes (exophthalmia)
- Feeling of sand in the eyes.
- Pressure or pain in the eyes
- Swollen or retracted eyelids
- Red or swollen eyes
- Sensitivity to light
- Double vision
- Sight loss
- And also, Graves dermopathy
A rare manifestation of Graves ‘disease, called’ Graves ‘dermopathy,’ is redness and thickening of the skin, most often on the shins or the tops of the feet.
What are the Risk Factors of Graves’ Disease?

Although anyone can get Graves disease, several factors can increase your risk of getting it. And also, these risk factors are as follows:
1. Family Background
- Because a family’s past of Graves’ disease is a known risk factor, there is a chance that one or more genes will make a person more prone to the disorder.
- And also, sex women are much more suitable to get Graves’ disease than men.
2. Age
- Graves disease usually occurs in people under 40 years of age.
3. Other Autoimmune Disorders
- People with other immune system disorders, such as type 1 diabetes or rheumatoid arthritis, are at higher risk.
- And also physical or emotional stress. Stressful life events or illness can trigger Graves’ disease in people with a genetic predisposition.
4. Pregnancy
- Recent pregnancy or childbirth can increase the risk of suffering from the disorder, particularly in women with a genetic predisposition.
5. Smoke
- Smoking cigarettes, which can affect the immune system, increases the risk of Graves’ disease. And also, smokers with it are at higher risk for Graves’ eye disease.
Complications of Graves’ Disease
Complications of Graves’ disease can be:
1. Problems During Pregnancy
- Graves’ disease’s possible complications during pregnancy are miscarriage, premature delivery, fetal thyroid dysfunction, low fetal growth, maternal heart failure, and preeclampsia.
- Preeclampsia is a maternal disorder that causes high blood pressure and other severe signs and symptoms.
2. Heart Disorders
- Graves’ disease can conduct heart rhythm disorders, changes in the heart muscles’ structure and function, and the heart’s inability to pump enough blood to the body (congestive heart failure).
3. Thyroid Crisis
- The thyroid crisis is a life-threatening but rare complication of Graves’s disease. It is also known as “accelerated hyperthyroidism” or “thyrotoxic crisis.” It is more likely when severe hyperthyroidism does not treat improperly.
- The sudden and drastic grow in thyroid hormones can cause several effects, such as fever, heavy sweating, vomiting, diarrhea,
- Delirium, severe weakness, seizures, very irregular heartbeat, yellow eyes, skin (jaundice), external blood pressure, and eat. The thyroid crisis requires immediate urgent medical attention.
4. Fragile Bones
- Untreated hyperthyroidism can also lead to weak and brittle bones (osteoporosis). The strength of bones depends, in part, on the amount of calcium and minerals they contain.
- Too much thyroid hormone affects the body’s ability to get calcium into the bones.
How is Graves’ Disease Treated?
These treatment options are available for people with Graves’ disease. And also, your doctor may propose you use one or more of these options to treat this disease:
1. Anti-Thyroid Drugs
- Anti-thyroid drugs, like propylthiouracil or methimazole, may prescribe.
- Beta-blockers may also use to help lessen the effects of your symptoms until other treatments begin to work.
2. Radioiodine Therapy
- It is the most common treatment for Graves’ disease. This treatment needs you to take doses of radioactive iodine-131.
- It usually requires you to swallow little amounts in pill shape.
- And also, your doctor will speak to you regarding any safeguard you have taken with this therapy.
3. Thyroid Surgery
- Although thyroid surgery is an option, it uses less often. Your doctor may recommend surgery if old treatments do not work correctly, if thyroid cancer suspects, or if you are a pregnant woman who can’t take anti-thyroid drugs.
- If surgery is necessary, your doctor may remove your entire thyroid gland to eliminate the risk of hyperthyroidism returning.
- You will need thyroid hormone replacement therapy on an ongoing basis if you opt for surgery. And also, speak with your doctor to learn more about the benefits and risks of different treatment options.
When to See the Doctor
Several diseases can cause the signs and symptoms associated with Graves’ disease. And also, check your doctor if you have any issues related to Graves’ disease for a quick and accurate diagnosis.
Seek urgent care if you have heart-related signs and symptoms, such as a fast or irregular heartbeat or experience loss of vision.
Conclusion
Graves disease is the leading cause of primary hyperthyroidism worldwide.
The case we have reported meets both clinical and analytical criteria to classify this patient with the diagnosis of primary hyperthyroidism due to Graves Basedow’s disease.
It is essential to clarify that the thyrotoxic condition was exacerbated in the postpartum period, as described in our patient’s literature.
Hence, doctors’ importance is to know incidence, clinical characteristics, treatment, and its main complications, one of the most important being Orbital ophthalmopathy with significant sequelae.